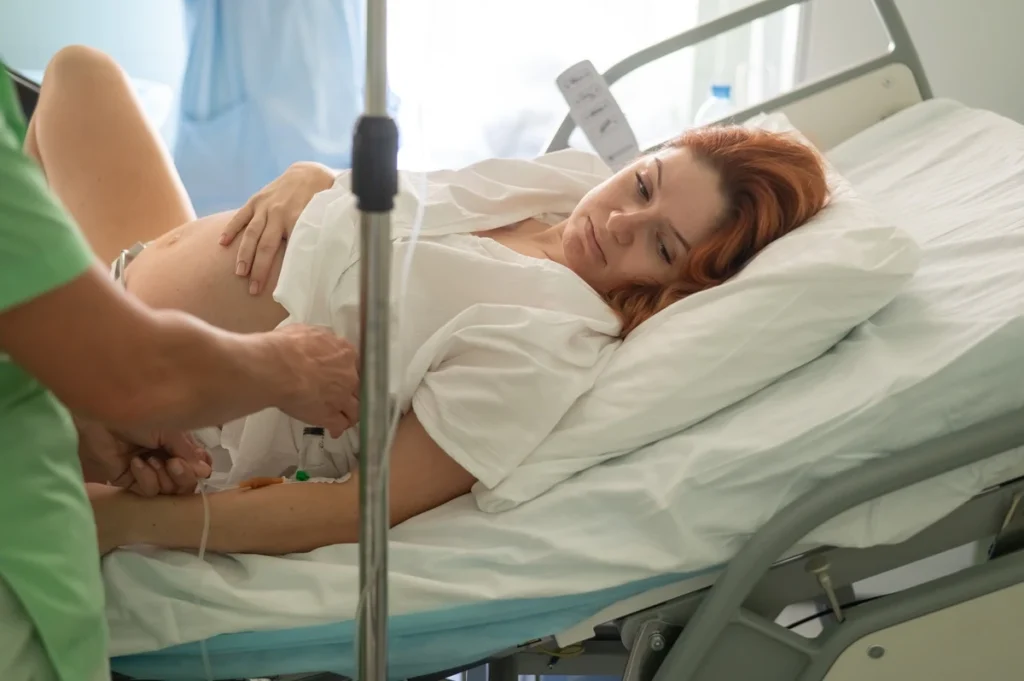
Poland introduces new policy allowing “birth rooms” as alternative to maternity wards in areas over 25km from specialized facilities.
What is a “birth room” and how does it differ from a maternity ward?
The regulations do not create a new “maternity ward.” They describe a service provided in a hospital with an admission room or emergency department, in a designated space for providing services with direct access to a full sanitary node. The goal is to ensure midwifery care and safety in emergency situations when childbirth begins outside the reach of an available maternity ward.
When should a “birth room” be used instead of a maternity ward – the 25 km threshold
This solution applies in areas where the distance to the nearest provider of obstetrics and gynecology services in a hospitalization setting exceeds 25 km. An additional condition is that the service must be provided in a hospital that has an emergency department or an admission room in its structure.
The new regulations will primarily affect regions where maternity wards are being suspended or closed and where there are accessibility issues.
The most important change: transport must be available “immediately”
The regulation directly requires 24/7 access to appropriately equipped transport if it becomes necessary to transfer the pregnant woman to a maternity ward. The transport means must meet two conditions simultaneously: it must be dedicated to such situations, not dependent on the current availability of the rescue system.
What must a “birth room” have to ensure a safe birth
The requirements for equipment of “birth rooms” are detailed. At the place where the birth is received, there must be elements enabling monitoring of the condition of the woman and newborn and carrying out basic rescue activities. The elements mentioned in the regulations include monitors, resuscitation equipment, and medications.
Additionally, birth kits are required, which must also be available in transport.
Who will be with the pregnant woman and who will travel in transport
The model is based on the midwife as the key person providing the service. The hospital must ensure 24-hour care by at least one midwife at the place where the service is provided. The midwife must have documented training in newborn cardiopulmonary resuscitation.
In case it becomes necessary to transport the woman to a maternity ward, transport is to be carried out by a team consisting of a midwife and an appropriately equipped ambulance.
What happens on-site when childbirth begins suddenly
The scope of the service includes actions by the midwife related to the assessment and safety of the patient and child. The regulations indicate, among other things, monitoring vital signs, pain management, and preparing for potential complications.
When the newborn will be transferred to specialized transport
The regulation contains indications that require the newborn to be transported by a “N” type (neonatal) team. The indications include prematurity, low birth weight, respiratory distress, or signs of neurological impairment.
In such situations, the regulations provide for the implementation of specialized transport, not standard transport.
How this will work in practice – three birth scenarios
Scenario 1: Onset of labor and there is time for safe transport. The midwife assesses the patient’s condition and decides on further management. If the condition and progress of labor allow, transport to the maternity ward is initiated.
Scenario 2: Labor is advanced and transport would be risky. Then the provider is obliged to accept the birth in the place where the service is provided, under the conditions provided for in the regulations (equipment, personnel).
Scenario 3: The newborn requires specialized care. If indications mentioned in the regulations occur, transport should be carried out by an “N” type team.